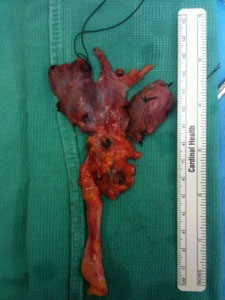
Cancerous Thyroid
Generally, well-differentiated thyroid cancer is indolent in nature and slowly progressive. It uncommonly represents a risk to the patient’s life if treated in a timely and appropriate manner. It is one of the most treatable and curable cancers. Surgery is the primary treatment. Sometimes, after surgery, treatment with radioactive iodine is indicated. Chemotherapy and radiation therapy, which are common therapies in other cancers, aren’t often used in well-differentiated thyroid cancer.
While we understand a lot about how thyroid cancer occurs, we don’t usually know why one person gets it and another person doesn’t. Thyroid cancer is more common in women than men. There is a significant increased risk of thyroid cancer in people who have been exposed to radiation at high levels. An example of this would be those who may have received radiation therapy to the head and neck for treatment of lymphoma. Simple x-rays, CT scans and MRIs don’t increase the risk of thyroid cancer. People with a family history of thyroid cancer, familial polyposis of the colon, and those with a personal history of breast cancer or Hashimoto’s thyroiditis may also be at increased risk. The best way to diagnose thyroid cancer is a fine needle aspiration (FNA) of the nodule in question.
When we talk about thyroid cancer, we are generally referring to well-differentiated thyroid cancer. This group of cancers make up the vast majority of thyroid cancer. There are four kinds of well-differentiated thyroid cancer.
- Papillary Thyroid Cancer(PTC)
- Follicular Thyroid Cancer(FTC)
- Hurthle cell cancer (HCC)
- Medullary thyroid Cancer (MTC)
