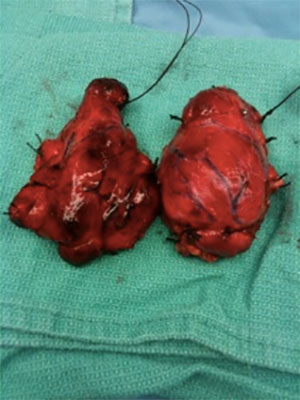
Grave’s disease (GD) is not typically considered a surgical problem in the United States. It is most commonly treated with radioactive iodine. We will discuss it on our website because it may be treated surgically in certain situations. The photograph above shows a typical example of a thyroid gland affected by Grave’s disease. The gland is, generally, diffusely, symmetrically enlarged. Nodules are minimal. The gland is highly vascular and over produces thyroid hormone leading to hyperthyroidism.
The typical patient is a young woman. Common symptoms include sweating, heat intolerance, palpitations, anxiety, and weight loss despite an increased appetite. Clinical findings include, tremor bulging eyes, and elevated resting pulse. GD is an autoimmune disease similar to Hashimoto’s thyroiditis. The immunology is complicated. Briefly, the immune system attacks the TSH receptors on the thyroid cell stimulating the thyroid gland and leading to enlargement and hyperthyroidism. Additionally, immune complexes may be deposited in the soft tissues behind the eyes leading to eye bulging ( exopthalmous) a common clinical finding in this disease. The diagnosis is made when a patient presents with a moderate diffuse goiter, low TSH and elevated Free T-4 and free T-3 levels. Most patients have elevated antibodies to the TSH receptor sites on thyroid cell membranes (Anti-TSH receptor antibodies).
Once the diagnosis is made the goal of therapy is to obtain normal thyroid function (a euthyroid state). There are three therapeutic choices:
- Antithyroid medication
- Radioactive Iodine therapy
- Surgery
Antithyroid medications include Tapazole and Propylthiouracil (PTU). These drugs directly inhibit the production of thyroid hormone. Over a period of 4-6 weeks the patient’s thyroid function returns toward normal. These medications represent the initial therapy for almost all patients. Some patients will stay euthyroid when the medication is stopped but most will redevelop hyperthyroidism if the medication is stopped. Up to 25% of patients will have issues with nausea and vomiting or skin rash. 1% of patients may have more serious issues with depressed white blood counts or liver problems. Antithyroid medications are not usually thought of as definitive therapy. Most commonly they are given to obtain a euthyroid state in anticipation of definitive therapy with RAI or surgery.
Radioactive iodine (RAI) is the most common form of definitive therapy in the U.S. Usually, an endocrinologist calculates a dose that is given by mouth as a outpatient. Over a period of weeks, the patient becomes euthyroid and then , commonly, hypothyroid. Typically, the patient has to go on thyroid hormone replacement therapy. RAI works very well. It’s advantage is minimal loss of normal activity and avoiding the risks of surgery. Disadvantages include a possibility of therapeutic failure; delaying pregnancy for at least 6 months after therapy and a theoretical risk of inducing a second malignancy. However, follow-up studies have not shown this to be true. It does not work well in large goiters. There is some evidence that it may actually worsen the eye issues common with the disease. Pretreatment steroids help minimize this problem.
Surgery is indicated in patients who have failed RAI or refuse RAI. It may be preferred in patient with worsening exopthalmous. It may be preferred in those with large goiters ( especially men) because of inconsistent results with RAI in this demographic. Surgery has the advantage of “instant” cure and no relapse potential . This approach does involve a period of recovery from surgery and a risk of voice compromise and/or hypoparathyroidism. The risks of these complications is about 1%. Some surgeons recommend subtotal thyroidectomy for GD with the hope that the patient will not need thyroid replacement therapy. However, subtotal thyroidectomy has a risk of recurrent illness if to much thyroid is left behind and it leaves the immune stimulus (the thyroid gland ) that can continue to contribute to worsening eye problems post-op. The operation has similar risks of complications as total thyroidectomy. If too much thyroid is removed the patient may still require thyroid hormone replacement therapy.
We usually recommend total thyroidectomy as definitive surgical treatment. After surgery, patients are treated with thyroid replacement therapy. A euthyroid state is generally readily accomplished. Total thyroidectomy removes the immune stimulus quickly and hopefully stops the progressive eye issues.
For surgery to be performed as safely as possible, patient are initially rendered euthyroid with anti- thyroid medications. On occasion, beta-blockers, such as propranolol, are prescribed if the pulse is too high. Typically, we prescribe SSKI for 7 to 10 days just before surgery. This is an iodine preparation. Giving it as described above is associated with safer surgery and better outcomes. Usually the patient takes 3 drops in juice three times each day. Also, we usually recommend a vitamin D-3 supplement ( 2000 IU each day) starting a couple of weeks before the surgery. This helps reduce issues with hypocalcemia post-op. The operation is completed as described on other pages. Same day discharge is typical. Throid medication is usually started a few days post-op.
