ANAPLASTIC THYROID CARCINOMA
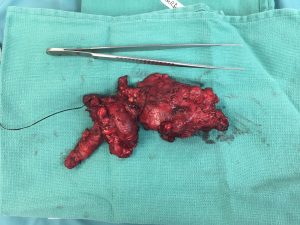
Anaplastic thyroid carcinoma is a rare, lethal form of thyroid cancer that primarily afflict elderly patients with untreated forms of differentiated thyroid cancer. It is thought that the accumulation of mutations over time ultimately leads to the changes that create this very aggressive and almost universally lethal form of thyroid cancer. Fortunately, this only comprises about 1.7% or all thyroid carcinomas, occurring in about 1-2 patients per 1,000,000.
The median length of survival for patients diagnosed with anaplastic thyroid carcinoma is 5 months. The 1 year survival is approximately 20% according to the 2012 American Thyroid Association Guidelines for Management of Patients with Anaplastic Thyroid Carcinoma, although this is possibly an overestimate.
Unlike differentiated thyroid cancers like papillary thyroid carcinoma and follicular thyroid carcinoma, anaplastic thyroid carcinoma has changed so much it does not resemble thyroid tissue at all, even when viewed under the microscope. Also, unlike management of differentiated thyroid cancers, the management of anaplastic thyroid carcinoma requires rapid diagnosis and treatment to obtain maximal benefit from therapy, as it grows very quickly.
The rarity and rapid progression to lethality has made development of treatment options difficult, as the coordination and implementation of plans from multiple providers can be a difficult task to perform quickly.
The first thing that needs to occur is for there to be adequate suspicion for this rare disease to warrant evaluation by a specialist that is familiar with this rare illness and can guide you quickly through the diagnosis and treatment options.
Signs and symptoms concerning for anaplastic thyroid carcinoma
- Age > 65; it is rare for patients to be younger than 50 years old
- Known or history of existing thyroid cancer like papillary, follicular, or Hurthle cell carcinoma
- New onset rapid enlargement of neck mass
- New onset or worsening symptoms of hoarseness, choking, pain, or difficulty breathing
Many other things can cause the above symptoms and are much more common. However, it is worth considering further evaluation if these symptoms persist or worsen despite standard treatment of the other causes, particularly if there is a neck mass associated with these symptoms. If there is enough suspicion of a rapidly progressive cancerous process, you will need imaging, diagnosis (by biopsy), and possibly surgery, radiation therapy, chemotherapy, or all of the above, based on how advanced the disease process is at diagnosis. It is best to establish the diagnosis in advance of surgery, but sometimes it is reasonable to proceed with surgery for diagnostic purposes.
You may require imaging in the form of ultrasound, CT scan, and PET scan before and/or after surgery. If you are a candidate for surgery, you will likely require laryngoscopy in advance of surgery to establish if your vocal cords are working normally prior to surgery. You may also be asked to undergo upper endoscopy or bronchoscopy to evaluate your esophagus or trachea for evidence of invasion prior to proceeding to surgery
The surgical procedure can be very extensive, including removal of any of the adjacent structures near the thyroid gland. These can include removal of parathyroid tissue, muscle, portions of the trachea, larynx, jugular vein, or other structures. You may require prolonged intubation or tracheostomy as a result of the surgery. You may require the placement of a feeding tube during or after surgery. The details of what may be required for removal, as well as a discussion of the relative benefit of extensive surgery, are individual decision points that depend on the extent of your disease and should be discussed with your surgeon prior to proceeding with surgery.
If the tumor can be removed without unreasonable morbidity, you will likely be offered radiation and/or chemotherapy after surgery. This is called adjuvant therapy.
Occasionally, if there is disease that will make surgery very difficult, you may be asked to undergo radiation and/or chemotherapy first, and then be reassessed for possible surgical removal. This is called neoadjuvant therapy.
More frequently, if the tumor is not surgically removable, you may be offered radiation and/or chemotherapy to try to slow progression of the disease around the neck and other distant sites. This is called palliative therapy.
There are many unique aspects of each patient’s disease such that any once care plan and recommendations will likely differ from another.
Regardless of any of the above scenarios, if diagnosed with anaplastic thyroid carcinoma, consultation with a palliative care specialist – a physician and medical team that specializes in reviewing end-of-life planning, is advisable due to the lethality and rapid progression. They will provide support and guidance, as well as a clear outline of the different things that can be done throughout the course of the illness.
